Osteoporosis: What It Is, Who’s at Risk, and How to Protect Your Bones
Osteoporosis: What It Is, Who’s at Risk, and How to Protect Your Bones
Osteoporosis is a common condition that weakens bones, making them more likely to break. It often progresses silently for years, and many people don’t know they have it until they experience a fracture from a minor fall—or even from bending, coughing, or lifting.
This blog covers the basics: what osteoporosis is, warning signs, risk factors, prevention steps, and treatment options.
What Is Osteoporosis?
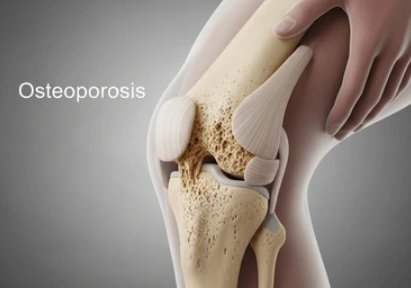
Osteoporosis literally means “porous bone.” Healthy bone is dense and strong. With osteoporosis, the body loses too much bone, makes too little bone, or both. The result is weaker bones that fracture more easily—especially in the hip, spine, and wrist.
Why It Matters
Fractures from osteoporosis can be life-changing. Hip fractures in particular can lead to surgery, loss of mobility, and long recovery times. Spinal fractures can cause chronic pain, loss of height, and a stooped posture.
Common Risk Factors
Anyone can develop osteoporosis, but risk increases with:
Age (risk rises significantly after 50)
Sex (more common in women, especially after menopause)
Family history of osteoporosis or fractures
Low body weight or small frame
Low calcium/vitamin D intake
Sedentary lifestyle
Smoking and heavy alcohol use
Certain medications, especially long-term steroid use (like prednisone)
Medical conditions that affect hormones or nutrient absorption (thyroid issues, celiac disease, etc.)
Symptoms and Warning Signs
Osteoporosis is often called a “silent disease” because bone loss happens without pain. Possible clues include:
Fracture after a minor bump or fall
Loss of height over time
Back pain (can be from a spinal fracture)
Stooped posture
If you have risk factors, it’s worth discussing screening even if you feel fine.
How Osteoporosis Is Diagnosed
The most common test is a DEXA scan, which measures bone mineral density. Results are usually reported as a T-score:
-1.0 or higher: normal
-1.0 to -2.5: osteopenia (low bone density)
-2.5 or lower: osteoporosis
Prevention: What Actually Helps
The best strategy is building strong bones early and protecting them as you age.
- Strength Training + Weight-Bearing Exercise
Bones respond to stress by getting stronger. Good options:
Walking, hiking, stairs
Resistance training (weights or bands)
Balance work (yoga, tai chi) to reduce falls
- Calcium and Vitamin D
Calcium supports bone structure.
Vitamin D helps your body absorb calcium.
Food sources (often best): dairy, leafy greens, fortified foods, canned salmon/sardines. Supplements can help if diet falls short—especially vitamin D in winter or with limited sun exposure.
- Reduce Fall Risk
Many fractures happen due to falls.
Clear clutter and loose rugs
Use good lighting
Wear supportive shoes
Get vision checked
Consider a balance routine
- Avoid Bone-Weakening Habits
Quit smoking
Limit alcohol
Review medications with your clinician if you’re at risk
Treatment Options
If osteoporosis is diagnosed, treatment is usually a combination of lifestyle + medication (depending on fracture risk).
Common medication categories include:
Bisphosphonates (help slow bone breakdown)
Denosumab (reduces bone resorption)
Anabolic agents like teriparatide/abaloparatide (help build bone)
Selective estrogen receptor modulators (SERMs) or hormone-related options in certain cases
The right choice depends on age, fracture history, kidney function, and overall risk profile.
When to Talk to a Clinician
Consider asking about osteoporosis screening if you:
Are a woman 65+ or a man 70+ (common screening ages)
Are 50+ with risk factors
Have had a fracture after age 50
Take steroids long-term
Have significant height loss or back pain without clear cause
Key Takeaway
Osteoporosis is common, serious, and often preventable—or at least manageable—when caught early. If you’re at risk, a simple screening test and consistent lifestyle habits can significantly reduce the chance of fractures later.
Related Links
